This article was co-authored by Trudi Griffin, LPC, MS. Trudi Griffin is a Licensed Professional Counselor in Wisconsin specializing in Addictions and Mental Health. She provides therapy to people who struggle with addictions, mental health, and trauma in community health settings and private practice. She received her MS in Clinical Mental Health Counseling from Marquette University in 2011.
There are 9 references cited in this article, which can be found at the bottom of the page.
This article has been viewed 21,548 times.
Menopause and perimenopause (the time when a woman's body is transitioning into menopause) can be an uncomfortable and stressful time in a woman's life. Perimenopause and menopause have similar symptoms, such as hot flashes and night sweats, irregular menstruation (until menstruation ends in menopause), vaginal dryness, mood changes, loss of bone mass, difficulty sleeping, slowed metabolism, and increase in cholesterol levels and weight gain. By incorporating a combination of medicines, self-care techniques, and lifestyle changes, perimenopause and menopause don't have to drastically alter your happiness or even your daily routine.
Steps
Coping with Hot Flashes and Night Sweats
-
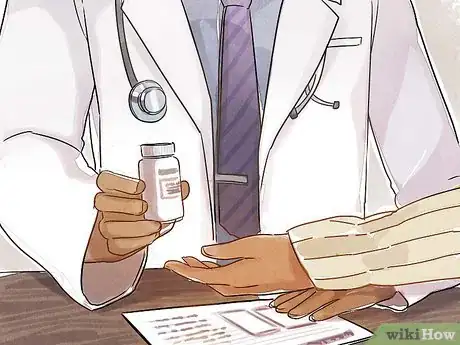
1Talk to your doctor about Hormone Replacement Therapy (HRT). HRT is the only FDA approved method for treating night sweats and hot flashes. It is effective, but some women choose to avoid hormonal methods of treating menopause because of safety concerns about taking hormones. Whether to use hormones is a personal decision.[1]
-
2Avoid known triggers of hot flashes. Known triggers of hot flashes are spicy foods, caffeine, alcohol, and smoking. Additionally, avoiding hot weather whenever possible will help with hot flashes. Skip the nightcap before bed and instead try ice water.[2]Advertisement
-
3Try adding soy to your diet. Although the research shows mixed results, some studies have found that the plant estrogens in soy can help ease hot flashes and night sweats, which are thought to be the result of decreased estrogen at menopause. Incorporate soy milk or tofu into your diet.[3]
-
4Incorporate moderate exercise. Upping your exercise routine can help stave off hot flashes. Though the reason for this is still being explored, it may have to do with the brain producing neurotransmitters like serotonin and dopamine, which can affect mood, sleep, and alertness.[4] Shoot for moderate exercise like 30 minutes of walking four days a week, and exercise indoors or avoid exercising outside during the hottest part of the day.
- In addition, exercising can help prevent weight gain and bone and muscle loss, which occur during menopause.
-
5Adjust your thermostat. If you feel hot, turn on the air conditioning or a fan until you find some relief. If you live in a space with no fan or air conditioning, taking a cool shower can also help with hot flashes.[5]
- Investing in bedding made of a cool, breathable fabric can help with night sweats. A satin blend or high thread count cotton sheets are great choices.
Preventing Vaginal Dryness and Painful Intercourse
-
1Be sure that your pain isn’t due to another condition. Painful sex can also be the result of other conditions like Endometriosis or Atrophic Vaginitis. Consult your doctor to rule out other causes for your dryness and discomfort.
-
2Talk with your doctor about estrogen replacements. If you’re experiencing pain during sex, you can ask your doctor about estrogen-infused gels or oral prescription medicines designed to help you lubricate naturally.[6]
- While these medicines are effective, they are not free from side effects. Weigh the pros and cons with your doctor to determine if these treatments are right for you.
-
3Try an over-the-counter lubricant. These lubricants will help replace your own natural moisture and lessen pain with intercourse. Options include one-time use lubricants and lubricant capsules that you insert into the vagina once or twice a week to proactively increase vaginal moisture. Be sure to choose a water-based lubricant and avoid oil-based lubricants like petroleum jelly.[7]
-
4Be sure you’re fully aroused before sex. It’s important to take your time and be fully in the mood for sex before you attempt intercourse. Foreplay is key. This will give your body time to create its own lubrication (as much as possible), which will minimize pain and dryness.[8]
-
5Don't feel obligated to engage in sex. If your body isn't cooperating, don't engage in painful sex. This conditions your body to expect intercourse to hurt, and this will do more damage, both physically and mentally, in the long run. Try again another time when you are in the mood and it doesn't hurt as much.
- Don't be embarrassed about this. Just as men sometimes need medication to obtain an erection, so too do women sometimes need medicines or extra lubrication to be able to have sex.
Easing Changes in Mood
-
1Join a support group. Finding support from other women who are going through the physical and mental changes can be comforting. Joining a group for menopausal women can also be therapeutic. In these groups women discuss coping strategies and approaches to dealing with menopausal symptoms that have worked for them.
-
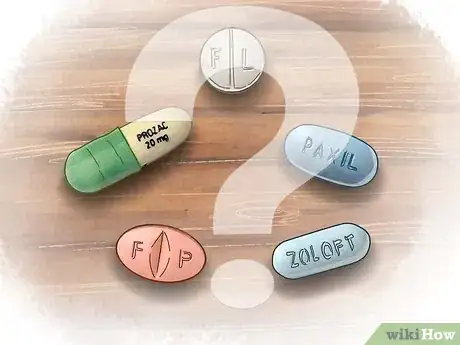
2Determine if antidepressants are appropriate for you. If your mood changes seem to go beyond the expected mood swings associated with menopause, talk to your doctor about whether you might benefit from an antidepressant. You might have depression, which is a serious condition, along with your menopausal symptoms.[9]
-
3Minimize stressors. Reduce stress in your life as much as possible. Incorporate yoga or meditation into your daily routine. Avoid overextending yourself socially or at work. If you're having an "off" day, take a personal day from work, if you have the leave time available to use.
-
4Practice self-care techniques. Even if you feel depressed or not like your normal self, it's important to do little things to make yourself feel better. Relaxation massages, facials, and manicures or pedicures are great ways to pamper yourself and give yourself a mental boost.
-
5Be sure to get enough sleep. Quality sleep is important for mental and physical health. Menopause can be exhausting, so it's especially important to get 7 to 8 hours of sleep per night.[10]
- Practicing good sleep hygiene techniques like turning off electronics and keeping your bedroom dark and cool will help you fall asleep more quickly and get better quality sleep. See this article for tips on how to Fall Asleep when You Can't.
Dealing with Erratic Periods
-
1Take a pregnancy test. In early stages of menopause transition, many women can still become pregnant. Double check that your erratic periods aren’t the result of an unexpected pregnancy. For extra peace of mind, check with your doctor as well, especially if you’ve been on a reliable form of birth control for a long time.
-
2Carry feminine hygiene products with you. When you can’t predict when or if your period will arrive, it’s important to be prepared. Be sure to carry tampons, pads, or a menstrual cup in your handbag so you aren’t caught in an uncomfortable situation.
-
3Download a period tracker app. The Apple Appstore and Google Play Store for Android have a wide variety of apps that help you track your periods and associated symptoms. If your periods become erratic because you’re entering menopause, these apps will help you know when your last period was and what symptoms you typically have at particular points in your cycle.
- These apps are especially helpful to document your symptoms so you can report specifics to your doctor. For example, if before each erratic period you tend to get migraines, a tracking app will help you pinpoint the specific dates you’re suffering each month so you can easily show these trends to your doctor.
-
4Pack painkillers in your purse or briefcase. If menopause-related headaches or migraines are common for you, it’s important to be proactive with your pain management, as these symptoms can be debilitating for many women. Acetaminophen, ibuprofen, and naproxen are good choices for over-the-counter pain management.[11]
- For stronger pain relief options, talk to your doctor about the extent to which your pain is affecting your everyday activities. Prescription treatments for migraines might be appropriate for you if over the counter treatments aren’t working, and you’re missing work or social events because of your pain.
-
5Bring a list of all your symptoms and be honest with your doctor. Your doctor can’t help you and give you the most accurate diagnosis if you withhold information from them. Some symptoms like vaginal pain or dryness can be uncomfortable to talk about, but remember your gynecologist is a healthcare professional who specializes in women’s health, so don’t feel embarrassed.
Expert Q&A
-
QuestionWhat not to eat or drink during menopause?
 Claudia Carberry, RD, MSClaudia Carberry is a Registered Dietitian specializing in kidney transplants and counseling patients for weight loss at the University of Arkansas for Medical Sciences. She is a member of the Arkansas Academy of Nutrition and Dietetics. Claudia received her MS in Nutrition from the University of Tennessee Knoxville in 2010.
Claudia Carberry, RD, MSClaudia Carberry is a Registered Dietitian specializing in kidney transplants and counseling patients for weight loss at the University of Arkansas for Medical Sciences. She is a member of the Arkansas Academy of Nutrition and Dietetics. Claudia received her MS in Nutrition from the University of Tennessee Knoxville in 2010.
Master's Degree, Nutrition, University of Tennessee Knoxville Master's Degree, Nutrition, University of Tennessee KnoxvilleExpert AnswerAvoid eating fried foods and foods that are high in fat and sodium such as processed meats and cheeses. Avoid eating simple sugars such as cookies, cake, and candy.
Master's Degree, Nutrition, University of Tennessee KnoxvilleExpert AnswerAvoid eating fried foods and foods that are high in fat and sodium such as processed meats and cheeses. Avoid eating simple sugars such as cookies, cake, and candy. -
QuestionWhat is good to drink during menopause?
 Claudia Carberry, RD, MSClaudia Carberry is a Registered Dietitian specializing in kidney transplants and counseling patients for weight loss at the University of Arkansas for Medical Sciences. She is a member of the Arkansas Academy of Nutrition and Dietetics. Claudia received her MS in Nutrition from the University of Tennessee Knoxville in 2010.
Claudia Carberry, RD, MSClaudia Carberry is a Registered Dietitian specializing in kidney transplants and counseling patients for weight loss at the University of Arkansas for Medical Sciences. She is a member of the Arkansas Academy of Nutrition and Dietetics. Claudia received her MS in Nutrition from the University of Tennessee Knoxville in 2010.
Master's Degree, Nutrition, University of Tennessee Knoxville Master's Degree, Nutrition, University of Tennessee KnoxvilleExpert AnswerAvoid drinking any sweetened drinks. Focus on unsweet drinks such as water, sparkling water, or unsweetened tea.
Master's Degree, Nutrition, University of Tennessee KnoxvilleExpert AnswerAvoid drinking any sweetened drinks. Focus on unsweet drinks such as water, sparkling water, or unsweetened tea.
References
- ↑ https://my.clevelandclinic.org/health/diseases_conditions/hic-what-is-perimenopause-menopause-postmenopause/hic-non-hormonal-ways-to-cope-with-hot-flashes-and-menopause
- ↑ https://my.clevelandclinic.org/health/diseases_conditions/hic-what-is-perimenopause-menopause-postmenopause/hic-non-hormonal-ways-to-cope-with-hot-flashes-and-menopause
- ↑ https://www.thewomens.org.au/health-information/menopause-information/managing-menopause
- ↑ https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4061837/
- ↑ https://www.nia.nih.gov/health/hot-flashes-what-can-i-do
- ↑ https://www.nia.nih.gov/health/hot-flashes-what-can-i-do
- ↑ https://www.nhs.uk/conditions/vaginal-dryness/
- ↑ http://www.ourbodiesourselves.org/health-info/vaginal-dryness-in-menopause/
- ↑ http://www.womenshealth.gov/publications/our-publications/fact-sheet/menopause-treatment.html

























































Medical Disclaimer
The content of this article is not intended to be a substitute for professional medical advice, examination, diagnosis, or treatment. You should always contact your doctor or other qualified healthcare professional before starting, changing, or stopping any kind of health treatment.
Read More...